
To access the carrier product and rate information provided by PRISM, check the box below indicating you have read and agree to the license agreement. A button will then appear to access PRISM.
This site uses cookies to track your agreement option. If the terms of the license agreement change or if you clear the cookies from your browser, this page will appear once again during the PRISM login process.
Why Choose Health Net?
✔ Lowest rates in the market – Affordable options without compromising quality.
✔ Robust PPO network – Competes with major carriers like Anthem and Blue Shield.
✔ Flexible HMO options – Networks to fit nearly every group statewide and every budget.
✔ Simplified underwriting – Only 25% participation required for groups with 5+ enrolling. No DE9C or prior carrier bill needed.
✔ Easy-to-sell benefits – $0 deductible HMO plans + four years of rate stability.
✔ Nationwide coverage – Cigna network access for out-of-state employees + state plurality rules for group qualification.
Start Including Health Net in Your Quotes Today!
Need guidance on networks, plan designs, or have questions? We’re here to help!
Call us at 800.696.4543 | Email us at info@claremontcompanies.com.
Login To PrismHelp your clients add value to their benefits program by offering employees coverage for their furry family members.
Keeping pets healthy and happy is a top priority. But even one unexpected trip to the vet can wreak havoc on an employee’s personal finances. And when a pet is ill or injured it can be stressful and distracting.
The long-term cost of caring for a pet will vary, but medical bills are inevitable. Finding the right pet insurance policy can help employees balance taking care of their furry family members with their own financial well-being.
With MetLife Pet Insurance coverage for dogs and cats, pet parents get reimbursed for covered unexpected expenses, so they can stay focused and productive at work.
Features Include:
How it Works:
Pet insurance is automatically added to new business and at the anniversary or renewal to clients (51-99 employees) with MetLife core coverage starting with March 1, 2021 business.
To learn more about this exciting value-add discount program, download the flyer and visit MetLife.
Why Pet Insurance Matters
Download the MetLife Pet Insurance Value Story flyer to learn more.
MetLife’s broad range of products and service solutions help provide income protection, maximize productivity, and minimize administration for employers of all sizes. Help your clients stand out from the competition with a more attractive benefits package.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
Get The Latest News with Text Messaging!
Your success is important to us, and we’re actively working on new solutions to support you throughout the year. To get the latest news via text messaging in the future, simply provide your cell phone number here.
Starting April 1, earn a $350 bonus for every Cigna + Oscar group with four or more enrolled employees. Effective dates from April 1, 2021 to December 15, 2021 are eligible. Learn more.
With Cigna + Oscar, your groups get quality care and all of these (EPO) plan features:
With rates comparable to Kaiser, and networks that include UCSF, Stanford, and Sutter, Cigna + Oscar brings together the power of Cigna’s nationwide and local provider networks, and Oscar’s member-focused tech-driven experience, to deliver small group health insurance that understands the unique needs of California small businesses and their employees.
To learn more about Cigna + Oscar, view our recorded webinar and web page.
Note: to enroll your groups, you will need to have an appointment with Cigna. Check out the Cigna + Oscar Appointments Guide for full instructions.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
According to the 2021 State of HR Survey, conducted by ThinkHR from October 12, 2020, to November 9, 2020, responses from 2,200 professionals revealed small-to-medium employers were still dedicated to the health and well-being of employees, even after a tumultuous year with countless human resource and compliance challenges.
ThinkHR’s 2021 State of HR Report dives into employers’ challenges with understanding and complying with laws and regulations that hindered their ability to focus on their employees, in addition to their need for help with complex issues and administrative burdens.
Gain more insights into what small-to-medium businesses are thinking this year by downloading the 2021 State of HR Report.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
Get The Latest News with Text Messaging!
Your success is important to us, and we’re actively working on new solutions to support you throughout the year. To get the latest news via text messaging in the future, simply provide your cell phone number here.
Due to the pandemic, dentistry has changed and the effects on how dental procedures are performed and access to care may be permanent. Below are the evolving trends and how Blue Shield of California is addressing this changing environment.
Dental Care Trends
Dental Provider Trends
How Blue Shield is Addressing These Trends
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
The passage of the Coronavirus Aid, Relief, and Economic Security (CARES) act on March 27, 2020 expands how you can use Flexible Spending Account (FSA) and Health Savings Account (HSA) funds. However, FSAs do not allow certain types of purchases, including the three mentioned below.
1. Masks
Even though recommended by the CDC, masks are an ineligible expense and cannot be purchased as an over-the-counter item using an FSA card. Learn more.
2. Multivitamins
Over-the-counter vitamins and supplements are not considered an eligible expense because of how the IRS determines eligibility. They are considered a dual purpose item and require a doctor’s note before purchasing. You’ll then need to submit a claim.
FSA funds can be used to purchase doctor-prescribed specific supplements with a Letter of Medical Necessity (LMN).
3. Weight Loss Items
When signing up for a weight loss program and purchasing items to support your health journey, you must have an LMN to back up your purchase. This includes scales, weight loss program costs, and supporting material such as training videos or online coaches.
If your pre-tax benefits are administered by BRi, have your doctor fill out an LMN. Otherwise, it’s best to not use your FSA funds for weight loss.
Visit the healthcare.gov website for eligible FSA expenses.
If you’re a Benefit Resource Inc. client, view the Eligible Expenses Table through your online account. The list contains a breakdown of items and their eligibility status. Just log in to BRiWeb and view the Eligible Expenses Table in documents.
To learn more, visit Benefit Resource Inc.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
Get The Latest News with Text Messaging!
Your success is important to us, and we’re actively working on new solutions to support you throughout the year. To get the latest news via text messaging in the future, simply provide your cell phone number here.
The Paycheck Protection Program (PPP) was reopened on January 11, 2021 with updated eligibility requirements and the possibility of a second loan for the hardest-hit small businesses. The new guidelines make it easier for businesses to obtain a first-draw PPP loan and a second-draw PPP loan to be used for eligible payroll and non-payroll expenses, including technology. Software and cloud upgrades, for example, are recognized as critical expenses, potentially including payroll, HR, and HCM platforms to digitize operations and support touchless, mobile-friendly solutions.
The PPP loan application deadline is March 31, 2021.
With the continued closures and operation restrictions, businesses have been forced to adapt and stretch resources to stay open. The good news, as of March 14, 2021, more than 7.8 million PPP loans had been approved, providing over $703 billion in relief. Unfortunately, lockdown and work-from-home measures brought about by COVID-19 have disproportionately affected small businesses – particularly in the leisure and hospitality sectors. And nearly a quarter of all small businesses (fewer than 500 employees), which employ roughly half of the country’s workforce, remain closed.
According to the Congressional Research Service, unemployment during the pandemic peaked in April 2020 at 14.8% and remained at a still-elevated 6.7% in December. With support from the Department of Treasury, the Small Business Association (SBA) originally began providing funds via the PPP program in March 2020 as part of the Coronavirus Aid, Relief, and Economic Security (CARES) Act. The Consolidated Appropriations Act of 2021 (CAA), signed into law in December 2020, provided an additional $284 billion in funding, referred to as PPP-2.
With so much of the workforce working remotely and the need to limit in-person contact, organizations dramatically increased the speed of adoption of digital technologies and converted manual, paper-based procedures to digital – from timecards, submitting receipts for reimbursement, and manual paycheck delivery, to taking customer orders. What’s more, many of these changes will be long lasting. According to a new McKinsey Global Survey, companies have accelerated the digitization of their customer and supply-chain interactions and of their internal operations by three to four years. In fact, technology’s strategic importance has become a critical component of business, not just a source of cost efficiencies.
This digitization investment will keep companies agile so they can respond to crises as well as evolve customer and employee demands. Cloud solutions offer key benefits that are critical for small businesses — like scalability, flexibility, cost, innovation, maintenance, and security.
PPP-2 funds can be used for both payroll and non-payroll expenses, including payroll costs, benefits, mortgage interest, rent, utilities, worker protection costs related to COVID-19, uninsured property damage costs caused by looting or vandalism in 2020, and certain supplier costs and expenses for operations, which includes payments for business software or cloud computing.
The following entities are eligible to apply for a First Draw PPP Loan through the latest wave of funding:
Second Draw PPP Loan Eligibility Requirements for Borrowers
Second Draw PPP Maximum Loan Amount
Second Draw PPP Full Forgiveness Terms
Second Draw PPP Loans made to eligible borrowers qualify for full loan forgiveness if during the 8- to 24-week covered period following loan disbursement:
To learn more, check out the Paylocity website.
Contact Claremont at 800.696.4543 or info@claremontcompanies.com for assistance when you’re ready to enroll a group in a Paylocity plan.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
According to the recently released Ease 2021 SMB Benefits and Employee Insights Report that focuses on the last three years (2018-2020), business decision makers are coping with healthcare increases by seeking ways to balance meaningful access and quality care with affordability. The report also offers a glimpse into how COVID-19 impacted SMB benefits, as well as shifted the way employees interact with their benefits.
With data collected from 2,000 health insurance agencies, 75,000 small businesses, and 2.5 million employees nationwide that use Ease, the Report found a continuation of the rise of healthcare costs and a sustained need to offer competitive total rewards packages, all while seeking new and innovative ways to contain mounting costs.
The Report Features Insights and Trends On:
Medical premiums for families and individuals continue to steadily rise, with rate increases eclipsing the rate of inflation for 2020. The average company in Ease saw an increase in individual medical premiums of 5.98%, while family medical premiums increased an average of 3.74%. These increases pose unique challenges to businesses as they try to contain costs while offering quality healthcare.
In 2020, companies that use Ease contributed an average of 73.97% to their employees’ individual medical premiums (down from 74.24% in 2019) and 59.12% to family medical premiums (unchanged for the past three years). This suggests that while premium costs continued to rise, employers’ costs remained fixed, passing the increase onto their employees.
Over the last three years, employers have reduced the number of medical plans offered by about 3%. By controlling and shrinking the number of medical plans available to employees, companies are able to steer their employees to selecting more affordable plan options, such as High Deductible Health Plans (HDHPs).
Voluntary benefits help supplement the gaps found in core medical plans, and are a smart way for companies to attract talent. Typically, the larger the company, the more voluntary benefit plans offered per employee. On average, the number of voluntary benefit plans offered per employee has increased by approximately 3% since 2018. The most popular plans are dental, vision, life, AD&D, and short- and long-term disability.
Businesses with:
Throughout 2020, during the pandemic, the key to small business survival is anticipation and adaptation. Small businesses forced to do more with less are in greater need of the right tools and technology to supplement tasks and activities previously handled by employees.
With the rise in unemployment and market volatility in 2020 as a result of COVID-19, certain industries were hit harder than others. The five hardest hit industries from a job loss and revenue perspective were hotels, sports and performing arts, furniture and home furnishing stores, restaurants and bars, and motion picture and sound recording.
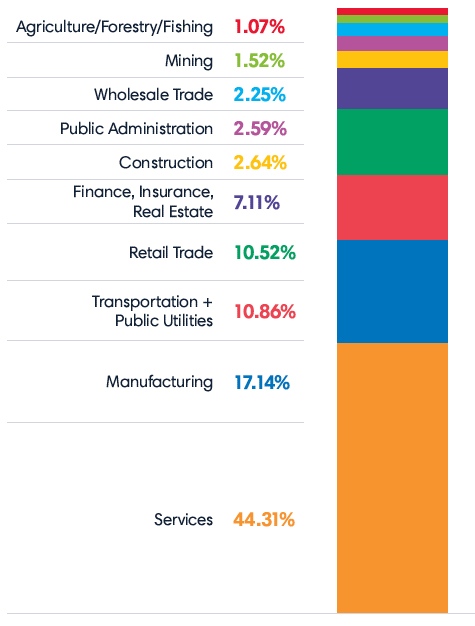
Of the 75,000 SMBs using Ease, the hardest hit industry was services (44.31%), followed by manufacturing (17.14%), and then transportation and public utilities (10.86%).
The largest category within the services segment is business services (47.87%), followed by health services (26.65%), and educational services (just under 10%).
In 2020, Brokers Helped Their Groups with The Following Activities:
Telemedicine rapidly became a necessity in 2020 and the number of employees enrolled increased 109% year-over-year.
Many of the 18 million furloughed workers returned to their companies in the second and third quarters.
To better understand the latest trends in healthcare and voluntary benefits, and advise your clients, download the Ease 2021 SMB Benefits and Employee Insights Report.
Ease is an online benefits enrollment system that makes it simple for insurance brokers and small business employers to set up and manage benefits, onboard new hires, stay compliant, and offer employees one destination for all their human resources information.
The Ease Marketplace is equipped with products, technology solutions, and resources to help you stay ahead of industry trends, defend against new competitors, and build a robust HR offering.
Don’t have an Ease account?
Contact us for free Ease online enrollment for your groups with one line of coverage or more.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
From February 2 to February 15, 2021, Blue Shield of California/Harris Poll surveyed 1,000 adults in California to gauge access to health care, comfort levels with workplace and public safety, and opinions of healthcare policy.
The Findings Include:
The poll represents Californians who are privately insured, uninsured, MediCal recipients, self-insured and more. It was conducted before Blue Shield of California was tapped by the State of California to oversee COVID-19 vaccine distribution as a third party administrator (TPA).
Access the article and infographic.
Access the Article and Infographic
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
Help your clients make the most of their accounts with the following tips and reminders.
Accountholders can make contributions to their 2020 plans until tax day 2021. View the video to learn how.
2021 HSA and High Deductible Health Plans (HDHP) Contributions and Out-of-Pocket Limits
Sterling’s Year-End Statement will show you how much is left to spend in your account and your deadlines for spending and reimbursement. To access your Year-End Statement, log in to your FSA account and view “Statements” then select “Year-End Statements.” Click “Run Statement” to generate a report showing any remaining funds left to spend for 2020, and any associated deadlines for associated spending and reimbursement.
The statement may include information on Rollover, Grace Period, or Run-Out Period. Below are the Rollover, Grace Period, and Run-Out-Period definitions.
Rollover
If your plan has a rollover, you may move up to $550 of unused FSA funds to the following plan year. The rollover doesn’t affect the following plan year’s maximum contribution amount.
Grace Period
If your FSA plan has a grace period, you have up to two-and-a-half months at the end of your plan year to spend unused FSA funds and incur new FSA eligible expenses. For example: If you had a December 31 FSA year deadline, your grace period would allow you to use your FSA funds through March 15.
Run-Out Period
If your FSA plan has a run-out period, you have an extended period of time at the end of the FSA plan year to submit receipts for reimbursement. You can only get reimbursed for claims incurred during the previous FSA plan year. The run-out period varies with each plan.
For more FSA information, visit the Sterling Administration website.
Take the guesswork out of what is eligible with your FSA and HSA plans with Sterling Administration’s partner – the HSA Store and FSA Store. It’s an easy-to-use online shopping platform that offers 24/7 chat and online help.
Use these valuable coupons when shopping.
Questions?
Contact your Claremont team at 800.696.4543 or info@claremontcompanies.com.
Please join us in congratulating Laura Hogsed and Karlee Navarro on their recent promotions, each to the new position of Assistant Manager, Service Team. As Assistant Managers, Laura and Karlee will be instrumental in helping clients receive the best service possible. They will assist in resolving complex matters, will manage workflow, and will solicit feedback from clients to improve on or develop new services while helping fellow team members realize their professional growth goals.
With over 20 years’ experience in the healthcare industry (seven years with Claremont) and with extensive knowledge of pharmacy benefits, Laura brings a wealth of knowledge to her new role. She is one of the most well-rounded members of the service team; if Laura does not have the answer (and that is rare) she can find it quickly. Laura enjoys the respect of everyone she works with, from clients to partners to teammates. We congratulate Laura on her promotion!
Karlee is the newest member of our service team, joining Claremont in 2020, and she has quickly made her mark. Karlee brings extensive experience from the brokerage side of the business where she managed a service team and a book of business while assisting producers as they pursued new opportunities. Karlee has deep knowledge in group benefits, understands and appreciates the broker’s and account manager’s perspectives, and has that unique “calm in a crisis” attitude that allows her to successfully work through the most challenging issues. We congratulate Karlee on her promotion!
You can reach Laura at laura@claremontcompanies.com or 925.296.8823 and Karlee at karlee@claremontcompanies.com or 925.296.8816.
Get The Latest News with Text Messaging!
Your success is important to us, and we’re actively working on new solutions to support you throughout the year. To get the latest news via text messaging in the future, simply provide your cell phone number here.